- Home
- Skin Yeast Infections
Skin Yeast Infections, How To Diagnose & Treat Them
Table of Contents
Updated 7/16/2023
Medically reviewed by Dr. Atmika Paudel, PhD - Written by Dan Jackowiak Nc, HHP and Dr. Shalaka Samat, PhD
Dr. Atmika Paudel, PhD who says... The information provided in this article about the causes, symptoms and treatments for skin yeast infections is medically correct.
Skin yeast infections were first discovered and classified in 1839 by
German professor of medicine Johann Lukas Schoenlein. The causative fungus in that case was a dermatophyte and was
later named Trichophyton schoenleinii that causes ringworm. This was the first microorganism
shown to cause infection or disease in humans.
In 1925, B.
Shelmire discovered skin yeast caused by candida and published his
findings in Arch. Dermatol. Syph. 12. Since then these candida skin
infections have been the topic of many research papers and studies.
The infections usually fall under three classifications:
1. Superficial infections caused by yeasts that have the ability to use keratin for food in the skin, hair, and nails.
2. Skin infections that happened because of a traumatic event and the yeasts were able to colonize the associated site.
3. Life threatening systemic yeast infections that are often seen in immunocompromised individuals.
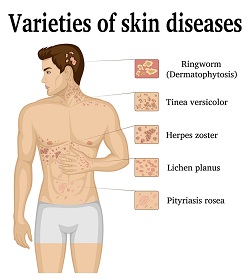
Most of these infections are caused by dermatophytes that are further classified as either Epidermophyton, Microsporum, and Trichophyton species. These yeasts are further sub-classified under these main species into approximately 40 other subspecies at this time. Most of these classified pathogenic fungi fall under the tinea subspecies.
According to C. C. Kibbler; jock itch, toenail fungus, dandruff, athlete's foot, and ringworm, are most often caused by one of the dermatophytes and infect 10 to 15% of the entire worlds population.
The basidiomycete fungi in the
genus Malassezia can also cause dandruff,
atopic dermatitis, eczema, ringworm, athlete’s foot, jock itch, and
nail infections (onychomycosis). Infants cradle cap is typically caused by Malassezia as well.
Causative factors for dermatophyte infections are most often associated with animals, especially cats, public swimming pools and public baths.
Dr. Shalaka Samant, PhD says...
Different fungi including Malassezia, Cryptococcus, Rhodotorula, and Candida species have been identified as human skin commensals. In healthy individuals, 11 out of 14 skin sites show a predominance of Malassezia species colonising them (1).
1. Topographic diversity of fungal and bacterial communities in human skin. Nature. 2013 Jun 20;498(7454):367-70. doi: 10.1038/nature12171. Epub 2013 May 22.
In healthy individuals, Candida albicans and Candida tropicalis are rarely associated with skin yeast on areas of the skin that are free of hair. In these areas, Candida guilliermondii and Candida parapsilosis are most often the culprits.
In areas where skin meets, such as the folds of the skin, or where there is high heat and moisture, Candida albicans is the most prevalent infectious yeast.
Skin yeast infections have been linked to elevated blood cholesterol levels. For instance when toenail fungus was treated, cholesterol levels were reduced. (British Medical Journal--1995) This of course would mean the fungus contributed to the high cholesterol.
Professor A.V. Costantini, former head of the WHO, found that cholesterol binds fungal mycotoxins in the blood stream as an immune system response to these toxins. Since it is possible that elevated cholesterol might be a result of the body defending itself against a fungal infection, getting rid of the fungus could potentially reduce the lipid levels too.
People with infections of the lungs have been found to suffer from skin yeast. Some may even resemble skin cancer. (C. C. Kibbler) Candida albicans can cause diaper rash and perleche, dry red skin or cracked skin at the corners of the mouth.
Dr. Shalaka Samant, PhD says...
Under conditions of immunodeficiency however, fungal diversity, and more importantly, the abundance of opportunistic species such as Candida on the skin increases (2). Fungal skin pathogens can be divided into two classes: dermatophytes and yeast, with Candida species belonging to the latter. Among the 200 known Candida species, only a few, including C. tropicalis, C. parapsilosis, and C. orthopsilosis, commonly found on healthy skin, can become pathogenic (3). C. albicans is the Candida species most often responsible for symptomatic skin infections (4).
2. The altered landscape of the human skin microbiome in patients with primary immunodeficiencies. Genome Res. 2013 Dec; 23(12): 2103–2114. doi: 10.1101/gr.159467.113
3.
Distribution of Candida Species in Different Clinical Samples and Their
Virulence: Biofilm Formation, Proteinase and Phospholipase Production: A
Study on Hospitalized Patients in Southern India. J Glob Infect Dis. 2011 Jan-Mar; 3(1): 4–8. doi: 10.4103/0974-777X.77288
4. Epidemiological trends in skin mycoses worldwide. Mycoses. 2008 Sep;51 Suppl 4:2-15. doi: 10.1111/j.1439-0507.2008.01606.x.
Other skin diseases like psoriasis, acne, hives, and eczema don't seem to have any relation to an internal fungus infection. But when people are treated for a fungal infection that have these other skin diseases, their external skin problems often go away. There are many studies showing that psoriasis can be caused by a fungal infection by either the fungus itself or their mycotoxins being released into the blood stream. (A.V. Costantini 1994)
The skin is the largest organ in the body. It protects your insides from the outside and more importantly keeps your insides from becoming outsides. It also can reveal many inside health problems because it does release toxins in the form of sweat from the body. Skin lesions and unexplained rashes can be early indications of an internal yeast infection.
These common types of skin yeast infections can affect other parts of the body as well. For example, you may have a severe case of athlete's foot and break out in a rash on the palm of your hand. The fungus did this by releasing mycotoxins into the blood stream, and the mycotoxins affected the palm of the hand.
The internal problem is in most cases, preventable. Usually, it is caused by diet, antibiotics, steroids, birth control pills, or possible inhaling of fungal spores in the home through air conditioning systems or water damaged areas.
Diagnosing Skin Yeast Infections
The best way to go is to take a skin
scraping or biopsy and look at it under a microscope for the presence of
hyphae. Care must be taken to not cut the skin when the sample is
taken. To do so leaves the patient susceptible to the yeast entering the
blood stream, which can result in death.
Many, but not all, of
the dermatophytes are fluorescent. So if you run an ultraviolet light
over the infection and it glows, it's a dermatophyte fungi. However not
all of these types of fungi glow under ultraviolet light so this is not a
very accurate test.
Cultures can also be taken and grown in a
petri dish, then the growth can be examined microscopically for hyphae.
Although this method is very accurate, it can quite often take one to
three weeks for a large enough sample to grow.
Dr. Shalaka Samant, PhD says...
Common symptoms of Candida (5) skin infections include thickening of the skin, hyperkeratosis, and erythema. Candida skin infections appear to display a preference for closed, moist areas of the skin that constantly experience friction. Recurrent Candida infections of the skin and other mucosal surfaces are referred to as chronic mucocutaneous candidiasis. These typically occur in individuals with impaired immune function, following prolonged antibiotic treatment, or after an injury. The risk for Candida skin infections is also higher in patients suffering from psoriasis (6). This might be favoured by treatment of psoriasis with corticosteroids and other novel immune suppressors which affect the body’s antifungal responses.
5. Skin Immunity to Candida albicans. Trends Immunol. Author manuscript; available in PMC 2017 Jul 1. Published online 2016 May 10. doi: 10.1016/j.it.2016.04.007
6.
A Clinician’s Guide to the Diagnosis and Treatment of Candidiasis in
Patients with Psoriasis. Am J Clin Dermatol. 2016; 17: 329–336.
Published online 2016 Jul 19. doi: 10.1007/s40257-016-0206-4
Medications for Treating Skin Yeast Infections
Skin yeast infections that are caused by the Tinea subspecies
of dermatophyte, can be treated by using an oral dose of 500 to 1000mgs
of Griseofulvin. In severe cases, or in the event the tinea does not
respond to Griseofulvin, then Terbinafine, Itraconazole, or Ketoconazole
may be helpful.
In many cases Tinea can be treated topically
with creams instead of pills. The creams that have shown good results
include Haloprogin, Cyclopiroxolamine, Clotrimazole, Econazole, Miconazole, Terbinafine, Tolcicate, and Tolnaftate. You might have to
try different creams to find the one that works the best. In super
severe cases, a cream with a pill may be necessary.
Candida yeast
infections of the skin quite often respond best to Clotrimazole, Miconazole, creams containing Haloprogin, Nystatin, or one of the Imidazoles. Severe cases may require a prescription of Fluconazole, Itraconazole or Ketoconazole in addition to the cream.
Dr. Shalaka Samant, PhD says...
Topical therapies work well to rid the skin of topical fungi and yeasts (7). Azole drugs such as miconazole, clotrimazole, and ketoconazole are fungistatic i.e. they limit fungal growth whereas allylamine and benzylamine drugs such as terbinafine, naftifine, and butenafine are fungicidal- they actually kill the fungi. Often, topical application of azole drugs is preferred for C. albicans skin infection treatment. However, infections of hair follicles, nails, and widespread infections often require systemic treatments.
7. Kyle, A.A., Dahl, M.V. Topical Therapy for Fungal Infections. Am J Clin Dermatol 5, 443–451 (2004).
Treating Skin Yeast Infections Naturally
Below are the best natural products we have found for treating skin
yeast infections naturally without the sometimes uncomfortable side
effects of prescription drugs.
If you suffer from any kind skin yeast disease, it may be wise to take a look at your diet. Many times allergies to foods cause intestinal dysbiosis which affects the appearance of the skin. It is also possible that the skin yeast is actually being caused by an internal yeast infection or fungal infection and their mycotoxins.
For relief of the symptoms of a skin yeast, try aloe vera gel or oil of oregano diluted in olive or coconut oil. Try the mixture on an area of skin that is generally tougher than delicate areas to get the solution right so it does not burn your skin.
An older class anti-fungal that is getting great results for skin yeast is Gentian Violet. Gentian Violet is a safe alternative to Lotrimin and was used extensively before the advent of the azole drugs, more information here. One word of warning; Gentian Violet will stain your clothes purple. People have reported that spraying your clothes with hair spray or Zout stain remover before washing takes the stain out.
Organic Coconut Oil is a superb Candida yeast infection killer. Studies have found that organic coconut oil explodes the nucleus of the Candida yeast cell effectively killing it. It also provides much needed relief from the itch that's often associated with Candida skin yeast infections. Just rub it on the affected areas like you would any lotion.
Cinnamon Oil was found to be deadly to oral thrush when applied directly to the lesions in AIDS patients. Because of this it also works very well for skin infections. You might have to dilute it like you do with oregano oil.
Grapefruit seed extract in liquid form
may also work. It always tests well on yeast species in the intestine
so should work well for treating skin yeast. This may have to be diluted
as well.
People are having very good luck with Terrasil Anti-Fungal Treatment MAX skin cream. Terrasil works very well for ringworm and tinea. It also helps relieve the itch and burning associated with these infections. A proprietary formula of minerals also promotes healing of the skin. This would be very good to use with the 11-strain probiotic powder.
Kolorex creams
active ingredient, horopito, has shown in numerous studies to be
effective against Candida. It can be applied directly to the infected
areas.
Lufenuron, commonly called cell wall suppressor or chitin synthesis inhibitor, has been medically proven to kill dermatophyte type of fungi that commonly infect the skin as various species of tinea. Tinea includes ringworm, jock itch, athletes foot, nail fungus, dandruff, and other dermatophytes. It has been used for years for dogs and cats with this type of skin yeast with very good success. Studies have been done for aspergillus and it did not work. However, there aren't any published studies for Lufenuron and Candida infections in humans.
The 11-Strain powder when combined with the diet on this website is showing fantastic results for unexplained skin rashes caused by whats going on in the gut that external treatments don't resolve. Some of these conditions people had for years and they are going away in weeks.
Dr. Shalaka Samant, PhD says...
It is being increasingly believed that modulation of Candida infection of the skin is very likely highly influenced by skin commensals – whether the Candida will turn pathogenic or remain a harmless commensal appears to be governed by the composition of the local skin microbiome. Topical applications of probiotic bacteria have a direct effect at the site of application by enhancing the skin natural defense (8) barriers and this might prove useful for combatting skin yeast infections.
8. Impact of prebiotics and probiotics on skin health. Skin and Hair. Beneficial Microbes: 5 (2)- Pages: 99 - 107 Published Online: February 28, 2014
Medical Review by Dr. Atmika Paudel, PhD
The above article mentions in detail about skin infections caused by yeasts and natural ways to get rid of them. As mentioned in the article above, skin yeast infections are mostly caused by dermatophytes. Some dermatophytes have intrinsic property to give fluorescence, which can be used for diagnosis of such fungi (1).
Although skin yeast infections are not usually life threatening in the beginning, they are a nuisance and trouble our daily life well-being. If not treated on time, sometimes, they can invade further into the tissues, then into the bloodstream which is, then, fatal. Therefore, care should be taken if we suspect infections on the skin, hair, or nails. Chronic skin infections can lead to other several complications and associated problems, requiring long-term treatment and other interventions.
Most skin yeast infections are superficial, and we can directly observe what is going on with our naked eyes, and we can know as soon as there is a problem unlike internal problems which we know only after they show symptoms. In cases of skin infection, sometimes we do not have any symptoms, but we can see redness on the skin, or some other signs by our eyes and then can check on to find out the cause earlier, or to treat accordingly. Sometimes, a thorough wash with soap water might be enough, while sometimes we can use some home remedies with substances that are easily available in our homes or if not at home, at a nearby supermarket or a drug store.
As the article has already mentioned above, simple treatments with home-available substances can be aloe-vera, oregano oil, gentian violet, coconut oil etc. Aloe-emodin, which is found in aloe vera, has antifungal property against dermatophytes (2). Similarly, oregano oil has effect against biofilms of fungi (3); Gentian violet is one of the economical and effective antifungal and antibacterial agent (4), and coconut oil has superb antifungal activity comparable to ketoconazole (5).
When compared with other diseases, skin problems are easily detected, but they need proper diagnosis in order to have a accurate treatment timely.
1. Ye, F., Li, M., Zhu, S., Zhao, Q., & Zhong, J. (2018). Diagnosis of dermatophytosis using single fungus endogenous fluorescence spectrometry. Biomedical optics express, 9(6), 2733–2742.
2. Ma W, Zhang M, Cui Z, Wang X, Niu X, Zhu Y, Yao Z, Ye F, Geng S, Liu C. Aloe-emodin-mediated antimicrobial photodynamic therapy against dermatophytosis caused by Trichophyton rubrum. Microb Biotechnol. 2021 Jun 24. doi: 10.1111/1751-7915.13875.
3. Hacioglu M, Oyardi O, Kirinti A. Oregano essential oil inhibits Candida spp. biofilms. Z Naturforsch C J Biosci. 2021 Apr 29. doi: 10.1515/znc-2021-0002.
4. Pona A, Quan EY, Cline A, Feldman SR. Review of the use of gentian violet in dermatology practice. Dermatol Online J. 2020 May 15;26(5):13030/qt79g6z0cf.
5. Shino B, Peedikayil FC, Jaiprakash SR, Ahmed Bijapur G, Kottayi S, Jose D. Comparison of Antimicrobial Activity of Chlorhexidine, Coconut Oil, Probiotics, and Ketoconazole on Candida albicans Isolated in Children with Early Childhood Caries: An In Vitro Study. Scientifica (Cairo). 2016;2016:7061587.
Have Any Questions About Skin Yeast Infections?
Do you have any questions about skin yeast infections or yeast infections in general? Ask your question here or contact us using the contact page of this website. It is also always a good idea to talk to your doctor as well.
Questions From Other Visitors
Click below to see questions from other visitors to this page...
How do I clean my hands if they are in a cast? 




Hi. I am in a real predicament. About 10 days ago I broke both of my wrists. I have a history of mild to moderate psoriasis and was dx last year with dyshidrotic …
Skin Yeast Infection Testimonials
Hi Dan!
I feel great! I have been taking the yeast cleanse supplements
and keeping the diet minus that one slip up where I had the potatoes
and tortilla chips. Isn't it incredible that my body immediately
detected the foods that I shouldn't have been eating and that were
causing the problem I had in the first place?
I can't thank you enough for your help. I can't believe the fungus went
away. It is refreshing to look at my arms and not see millions of white
spots. It seems like a miracle.
Genuinely,
Caroline
*****
Hi Dan,
I wanted to let you know that I feel so good you have NO idea. I am not so tired all the time and I feel energetic and I can rise early in the morning. I thank God.
My partner has beautiful skin on his hands again, and his feet are cleared up. It is amazing that you know all this stuff and you can't even see us, unlike the doctors we have here who yet don't have a clue.
Well I wish you a great holiday and thanks so much for helping me. I will send you some pictures of the new happy me.
I really appreciate your time and efforts to assist me.
God bless you,
Bernice
*****
Hi Dan,
I just wanted to inform you that I have been doing your candida cleanse with a wellness formula for boosting the immune system and my skin has cleared up completely. After 6 months of no results from the doctors I have relief. I am going to follow up with more Biofase and Profase and continue to keep up with a better diet. Thanks Again For your time and please feel free to use my info to help others. I do think that the boils were caused by the a yeast or bacterial infection in my hair follicles.
Thanks Again
Chris K.
IN
*****
Dan,
I just wanted to write and let you know how much I really appreciate all the advice you have given me about my skin condition. I also have great news, I have been seeing a kinseologist who has been treating me for my rash. He is also a naturopathic doctor and has me taking a variety of herbs. My skin is better then it has ever been and is improving every week. I'm still eating very healthy and keep a positive attitude. I will always take your advice with me when considering my health and will never forget it. Thank you sooooo much from the bottom of my heart!
Sarah Hall
I knew Sarah was going to send a yeast infection testimonial like this since we communicated by email almost every day for a few months. She had this in her scalp so bad her hair was falling out. The hair started growing back after a couple months and I am glad to see she is continuing with an aware doctor.
*****
Hi Dan,
I love your newsletters and I am slowly getting there with an
improvement in my health, I think my problem was a yeast infection of
the skin. I own my own restaurant so bar-tending 6 nights a week for two
years has had an affect. I'm sure a simple fungal infection went crazy,
then stupid Dr's messed me up with 5 different anti-biotics and now I'm
following your dietary advice and the bacterial products too are
finally working. Thank you so much my hands and big toe were the victims
here, and I'm finally seeing improvement. Awesome website and logical
information, really appreciate your help.
Yours Sincerely,
Fay
*****
Hello Dan,
I have used your Biofase product a number of times now and have found it very effective in removing dermatitis from my face and ringing in my right ear due to yeast infection.
Kind Regards,
James
*****
Hi Dan,
Your wonderful website and newsletters have helped me immensely, my skin
candida is gone, it's been gone for a while without any indications of
recurrence. I feel a lot better, most of the symptoms are gone, I
haven't done any testing yet, but I will very soon. I had a great side
effect, I lost so far 22 Lbs and I hope to lose more, because my eating
habits have changed, no more sugar or flour for me, a small price to pay
for feeling well and looking a lot better.
Thank you so much for sharing your knowledge, I really, really appreciate it.
Sincerely,
Cristina
Skin Yeast Infections & Yeast Infection Advisor Home
Home Privacy Policy Copyright Policy Disclosure Policy Doctors Store
Copyright © 2003 - 2025. All Rights Reserved under USC Title 17. Do not copy
content from the pages of this website without our expressed written consent.
To do so is Plagiarism, Not Fair Use, is Illegal, and a violation of the
The Digital Millennium Copyright Act of 1998.