- Home
- Candida Structure
Understanding the Structure of Candida, Yeast, and Fungi
Table of Contents
Updated 12/05/2022
Medically Reviewed by Dr. Vibhuti Rana, PhD - Written by Dan Jackowiak Nc, HHP and Dr. Atmika Paudel, PhD
Dr. Vibhuti Rana, PhD says... The information presented here about the structure of Candida yeast biofilms and their cell structure is medically correct.
We must understand the structure of candida, yeast, and fungi in general to successfully treat the condition. It truly is its own life form being partly vegetative, partly animal, and partly bacterial in nature. It is this ability to adapt and change form, or shape shift, that causes it to be so hard to eradicate from the human body. Once we understand its composition, then we can successfully treat it by natural methods that are safe without damaging the body.
The Structure of Candida Yeast Biofilms

Yeast usually lives within the intestinal environment of the human body and usually causes no problems.
But due to various environmental factors (see Cause) it switches to an
invasive multi-cellular form known as Candida from a unicellular or yeast
form and begins to reproduce very rapidly. As it spreads it builds a biofilm much like Helicobacter pylori does as a means of protection. These biofilms can range from 25 to 450 μm in thickness and begin to appear within the first 24 hours of colonization.
The fungal biofilm is composed of cellulose plant matter, polynucleotides that are primarily its DNA and RNA material, polypeptide proteins, and polysaccharide carbohydrate glucans. It also contains lipids or fats. The biofilm also contains fibrinogen and fibronectin which is used as an anchor material and is the same material that the body uses to clot the blood at wound sites. These materials are bound together by lignans with properties of stickiness, much like lectins in wheat. To keep it simple, proteins make up 55% of the biofilm, followed by carbohydrates at 25%, lipids or fats are 15%, and nucleic acids are 5%.
The biofilm may
also contain spores, hyphae, and pseudohyphae if the specific species of
yeast produces them. In the species that don't produce hyphae and
pseudohyphae but only produce spores or buds, these spores may found in
the biofilm as well. Occasionally, these spores or buds will be released
into the host as the yeast tries to spread.
One structure of
invasive Candida grows as a smooth white colony, and one grows as a rod
like flat gray colony. These colonies can be either smooth or wrinkled
too. This can be the same species of Candida and it can switch between
the phases as a method of adaptation. Candida tropicalis is known
to undergo switching or as I like to say, shape shifting, and produces
seven different types of colonies. This switching ability is reversible
and is inherited from one generation to the other. Research has also
shown that structural chromosome rearrangements are a way to maintain
genetic diversity and is an adaptation strategy of this species of
fungi.
Candida
hyphae reproduce sexually since the nucleus has two copies of the
chromosomes to create two separate cells through the sporangia when a
male and female meet. If you could call it male and female, it really
isn't, it’s more like two cells splitting themselves to join and create a
new cell.
Yeast is the unicellular structure of Candida albicans before it becomes multi-cellular Candida and although there have been over 1000 species classified, only around 150 species can survive within the human body. Yeast can be either anaerobic or aerobic and in the absence of oxygen they produce their energy by converting sugars into carbon dioxide and ethanol, and you wonder why you have brain fog?.
They can reproduce asexually or sexually. During asexual reproduction, the cell basically divides as a new bud to produce a new yeast cell without producing spores in the gut. Spores are believed to be highly inconspicuous to the immune system, which is exactly what a low-profile resident of the gut would want to avoid.
Fungi are pretty fascinating when you think about it. Here we have a life form that is vegetative, animal, and bacterial in nature. The cell wall is composed of plant material and proteins, the membrane and nucleus are proteins and fats like an animal, and it reproduces like bacteria in many cases asexually while carrying only one set of chromosomes, depending on the species. It clones itself, and has the ability to shape shift and take seven different forms while rearranging chromosomes as an adaptive strategy to insure survival. No wonder it is so hard to get rid of!
Dr. Atmika Paudel, PhD says...
When Candida cells attach to a surface, they multiply while adhering together and are surrounded by extracellular polysaccharide matrix, this structure is called biofilm. Biofilms can be formed inside the body or in surfaces like catheters. As biofilm forms a matrix around the Candida cells, it protects Candida from recognition by the host immunity and from antifungal drugs by resisting the antifungal agents’ penetration (1). Thus , Candida cells can remain inside the host without being detected for a long time by forming the biofilms. Similarly, by restricting the entry of antifungal drugs, Candida cells survive and persist inside the host. In addition, biofilms can alter the cytokine production in the host to manipulate the host immune system. Therefore, biofilms are hard to treat.
1.
Christina Tsui, Eric F. Kong, Mary Ann Jabra-Rizk, Pathogenesis of Candida albicans biofilm, Pathogens and Disease, Volume 74, Issue 4, June 2016
The Basic Cell Structure of Fungi
Fungi belong to the group of organisms called eukaryotes that are organisms with complex cells in which the cell has a nucleus. Animals and plants share this center nucleus among their cell types, bacteria do not.
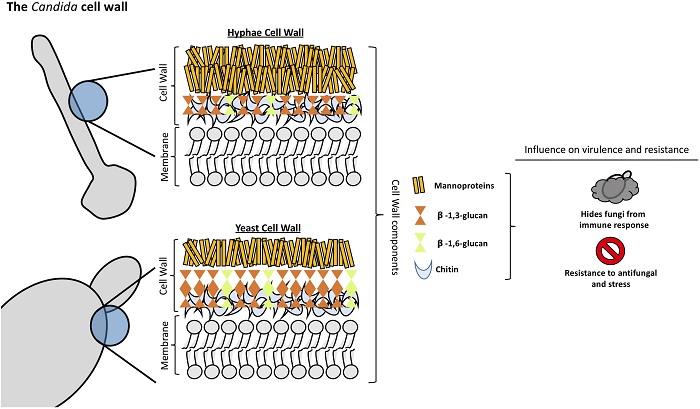
The cellular wall of fungi is composed of mannoproteins, glucans and chitin. Mannoproteins are highly glycosylated proteins. Glucans and chitin are vegetable in nature and what gives the cell its rigidity. The three combined nearly bears the same composition as that of vegetables. This helps them to stand upright and grow reaching for the sunlight. It is composed of one cell thick filaments that are often called hyphae and are very similar to roots of plants since fungi feed from these hyphae. These roots can puncture intestinal walls and organs in the human body creating leaky gut syndrome and other deteriorating effects.
Inside of cellular wall is a protein and fat membrane, also known as a lipoprotein membrane, which is the common cellular structure of animal and human cells. In the center is a nucleus and together with the lipoprotein membrane beneath the vegetative cell wall. The presence of the membrane makes them very similar to animal cells.
They reproduce asexually in many cases through the production of spores. They can also mate with other fungi when two mycelial hyphae, or sporangia meet, producing two multinucleate ball shaped cells that join together to form a new nuclei. Asexual division is very much like bacteria that simply split and each cell contains the same set of chromosomes although the prokaryotic bacteria have no nucleus. The fungal spores possess this dividing or splitting ability.
Fungi feed through the hyphae and spores produced by them, releasing exoenzymes into the surrounding substrates they adhere to in search of nutrition, mostly glucose. These enzymes act like digestive enzymes in animals; but they digest the substrate from the outside of the fungi, absorbing the broken down nutrient molecules through the cells. All fungi are decomposers with some species growing on dead organisms while some grow on, or within, living organisms as parasites.
In the case of vaginal Candida albicans infection, it becomes invasive by first puncturing the lining of the vaginal skin with its mycelial form possessing the hyphae. If the food supply is good it begins to produce spores that can double its population in an hour. If the food supply is lean then it sends out more hyphae in search of food.
Candida's primary food source is simple carbohydrates which it uses to produce carbon so it can grow. Candida albicans must have biotin, which is also known as vitamin B7 to grow. Other species like Candida glabrata must have niacin and pyridoxine or vitamin B6 but candida glabrata does not produce hyphae, only spores and is extremely resistant to Diflucan. Because of this resistance it is believed to be an adaptation to the drug.
Dr. Atmika Paudel, PhD says...
The article is very well written. The most impressing factor about the article is that it explains the yeast cell structure and biofilm structure in such a simple way that it is understandable by anyone. Scientists would use more complex sentences and scientific terms which may be unknown to many. The article says that Candida cell resembles in some points to bacteria, in some points to plant and in some points animals. Since Candida is eukaryotic, consists of chitin in the cell wall and can exist in different morphological forms, it is highly adaptable fungus. I will not be going in details about the cellular structure, which the article has already done beautifully, I would just add few important aspects regarding the structural importance in host-pathogen interaction.
All the three major components of the cell wall - mannoprotein, beta glucan and chitin are important for Candida to evade and escape the host-immune system to establish infection (1). The cell wall structures try to hide Candida from the recognition by host immune cells, thereby they escape the host immunity and survive inside the host body. In addition, the cell wall structures provide rigidity to the fungal cell, provide easy adherence to host tissues and also alter host macrophage nitric oxide production for less engulfment of the fungal cells.
(1) Garcia-Rubio, Rocio, et al. The fungal cell wall: Candida, Cryptococcus, and Aspergillus species. Frontiers in microbiology 10 (2020): 2993.
How Do We Get Rid Of Candida Yeasts & Fungi?
Since fungi are decomposers, the common speculation that it eats only sugar is a misnomer in my honest opinion. Yeast eats sugar and produces ethanol and carbon dioxide; yeast is the unicellular form. Candida is the multicellular form that sends out hyphae that feed by releasing exoenzymes into whatever it is attached to, or comes in contact with. This external digestion allows Candida to absorb the nutrients through the hyphae. Therefore, everything is a possible food source though it is mostly looking for glucose.
Generally, the highly acidic environment of the stomach will not allow Candida to live so it is found in the small and large intestine mostly. Some kind of colon cleansing product is most often needed so a person stays regular> This cleanse will help remove excess mucous from the top of the biofilm while helping to break down the biofilm itself, flushing it out and dislodging it from the intestinal wall.
Enzymes specifically designed to remove the biofilm and help digest the
polysaccharides, mannoproteins and chitin, i.e. proteins and carbohydrates
in the cell wall should now be introduced. This process will
expose the soft
lipoprotein membrane to destruction by medically proven natural anti-fungals.
Here is a testimonial for a fungal infection-treated satisfied person:
Hi Dan!
I have been battling Candida for 9 months, tried many products and even many trips to doctors. Biofase and Profase are the first products I have taken where I am noticing a change. WHY don't they educate you on the biofilms!!!!. Thank you for opening my eyes to that fact. I am going to be ordering more soon!!!!
Thank you!
Melissa
Most people that are infected with Candida suffer from immune system dysfunction whether they are aware of it or not. For instance, in vaginal yeast infections there have been studies suggesting a deficiency in T-lymphocyte responses that permit the Candida to take hold and allow its overgrowth.
So it would be best if we boost or stimulate immune system function, raise
antioxidant levels in the intestine, and in general provide the body with
good nutrition through supplementation and diet. The immune system
should also come into play and the macrophages, lymphocytes, and
neutrophils can begin to clean up the mess as they help destroy the
fungi. IgA levels can also be increased through supplement usage to increase protection and heal the walls and other mucous linings of the intestine.
In cases of chronic vaginal infections the hormones may have to be balanced since the yeast becomes hormone dependent as evidenced by the re-occurrence at particular times of the menstrual cycle. We know that it must have excess estrogen to survive and estrogen influences vaginal glucose levels.
Excess estrogen not only causes cancer, mostly breast, but also raises the glycogen levels in the vagina and glycogen is the food supply for yeast. If you suffer from bad pms symptoms the chances are you have high estrogen levels that need to be corrected. Your menstrual cycle should sneak up on with you with very little discomfort.
High cholesterol levels, plaque, scar tissue as in Fibromyalgia, etc, that are possibly created by the fungi, can be resolved with another special enzyme designed to digest these substances from within the body.
The Treatment Plan I suggest for fungi, Candida, and yeast addresses all these problems and the Candida has no natural defense against some of these products. They can't adapt and shape shifting doesn't help them either, they are totally defenseless, it is only a matter of time before you have won your battle with this beast!
Does any of this make sense to you?
If it does, take a look at the Yeast Infection Treatment page.
Medical Review by Dr. Vibhuti Rana, PhD
The information mentioned in the above article regarding the structure of Candida yeast is correct.
The Candida yeast has the biofilm making property, which makes it very difficult to be accessed and treated.
Biofilms are known as early as 1700s, when Antony van Leeuwenhoek discovered the same in his own teeth. Apart from bacteria, fungi such as Candida, Cryptococcus, Aspergillus, Pneumocystis, and Coccidioides also form biofilms.(1)
Studies have now shown that the surface filamentous fungi have the capability to form biofilms, which affects the host immunity, and standard of living.
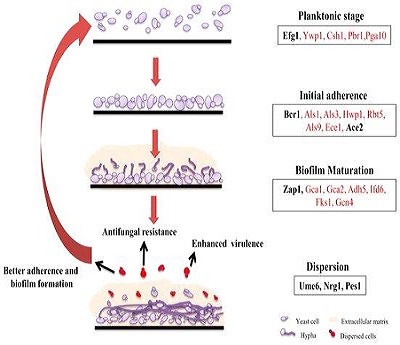
Harding et al, in 2009 proposed a model of the biofilm formation for filamentous fungi.(2) As can be seen from the image to the right, the main steps of biofilm formation are adhesion, proliferation, maturation, and dispersion.(3)(4) These growth phases transform the sticky, adherent blastospores to well-defined cellular communities or colonies, encased in a polysaccharide matrix. Experiments conducted using fluorescence and confocal scanning laser microscopy demonstrated that C. albicans biofilms have a highly heterogeneous architecture composed of cellular and non-cellular elements.
As we can well understand, antifungal resistance of biofilm-grown cells increased in conjunction with biofilm formation. A combination of the existing antifungal treatments with other drugs, probiotics, and hormone regulators, can be used as a therapeutic approach to treat biofilm-based infections.
- 1. The Significance of Lipids to Biofilm Formation in Candida albicans: An Emerging Perspective Alim et al., J. Fungi 2018, 4(4), 140; https://doi.org/10.3390/jof4040140.
- 2. Can filamentous fungi form biofilms? Trends in Microbiology, Volume 17, Issue 11, November 2009, Pages 475-480
- 3. Hawser, S.P.; Douglas, L.J. Biofilm formation by Candida species on the surface of catheter materials in vitro. Infect. Immun. 1994, 62, 915–921.
- 4. Chandra, J.; Kuhn, D.M.; Mukherjee, P.K.; Hoyer, L.L.; McCormick, T.; Ghannoum, M.A. Biofilm formation by the fungal pathogen Candida albicans: Development, architecture, and drug resistance. J. Bacteriol. 2001, 183, 5385–5394.
Have Any Questions About the Structure of Candida Yeasts?
Do you have any questions about Candida biofilms, its cell wall structure or yeast infections in general? Ask your question here or contact us using the contact page of this website. It is also always a good idea to talk to your doctor as well.
Questions From Other Visitors
Click below to see questions from other visitors to this page...
Are there phases or cycles of procreation of Candida? 




Hello Dan,
As most living organisms have cycles if not all, is there evidence of candida cycles that provide information on procreation? If so, is there …
Is there anything topical that would attack the biofilms, so I can kill a chronic fungal skin infection? 




Hi Dan, I have been struggling with a fungal infection that comes and goes for years. I do use your whole internal system, and my digestive system is in …
Yeast Infection Advisor Home & Structure of Candida Yeast Home
Home Privacy Policy Copyright Policy Disclosure Policy Doctors Store
Copyright © 2003 - 2025. All Rights Reserved under USC Title 17. Do not copy
content from the pages of this website without our expressed written consent.
To do so is Plagiarism, Not Fair Use, is Illegal, and a violation of the
The Digital Millennium Copyright Act of 1998.