- Home
- Find the Cause
- Estrogen Dominance
Estrogen Dominance & Recurring Yeast Infections
Updated 5/21/2021
Medically reviewed by Dr. Atmika Paudel, PhD - Written by Dr. Shalaka Samant, PhD and Dan Jackowiak Nc, HHP
Dr. Atmika Paudel, PhD says... The article correctly shows how high estrogen level can affect the vulnerability to yeast infections.
Estrogen dominance or excess estrogen is one of the primary causes
of recurring yeast infections. My hope is that this page will help you
understand how this can happen; what it can lead to, and how to fix it.
Excess estrogen will literally feed Candida growth because estrogen controls vaginal glycogen levels. This
is why birth control pills and estrogen replacement therapy put women at
a greater risk of developing Candida yeast infections.
Short of
testing, we can take a look at the symptoms of premenstrual syndrome and
determine if you suffer from estrogen dominance.
Symptoms of Too Much Estrogen
Dr. Katharina Dalton of the U.K., a leading specialist who first used the term "premenstrual syndrome" defines it as the presence of recurrent symptoms before menstruation with the complete absence of symptoms after menstruation.
PMS
differs from all other disorders because the diagnosis does not depend
on the type of symptoms you suffer from, but when your symptoms appear
and disappear.
Doctors have identified at least 150 symptoms
that occur in PMS, but fortunately, because all of us are different, no
one has all of them! Among the most common are bloating, headache,
backaches, severe grouchiness, depression, breast tenderness, loss of
libido and fatigue.
Do these symptoms sound familiar? They are symptoms of estrogen dominance!
If
you suffer from PMS every month, you are probably estrogen dominant.
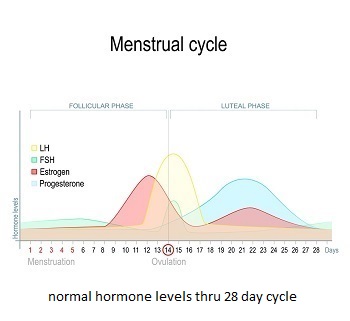
Either your estrogen levels are too high or your progesterone levels are too low, which has the very same effect because progesterone offsets the effects of estrogen. Your menstrual cycle, if your hormones were in balance, should sneak up on you with very few, if any, symptoms.
Estrogen levels also sky rocket when you are pregnant.
Dr. Shalaka Samant, PhD says...
The information provided in this article about estrogen dominance, its impact on other hormones, and its association with a greater risk of developing vaginal candida yeast infections is medically correct.
Vaginal candida infections are an important concern amongst all women of child-bearing age, with as many as 75% women having reported at least one episode (1) of such an infection during their lifetime. Although several factors, such as, excessive antibiotic use, immunosuppression, and diabetes are known to increase susceptibility to candida infections, the prevalence of candida colonization of the vagina has been observed to increase during pregnancy (2).
Several studies have found that pregnant women were more likely than non-pregnant women to experience a symptomatic infection caused by Candida species. Pregnancy-related factors, such as decreased cell-mediated immunity, increased estrogen levels, and increased vaginal mucosal glycogen production are believed to be responsible for providing a conducive environment for the infectious growth of Candida species.
1.
Vaginal colonization by bacteria and yeast. Galask, Rudolph P. American
Journal of Obstetrics & Gynecology, Volume 158, Issue 4, 993 - 995.
April 1988
2. Vulvovaginal candidiasis in pregnancy. Curr Infect Dis Rep. 2015 Jun;17(6):462. doi: 10.1007/s11908-015-0462-0. https://www.ncbi.nlm.nih.gov/pubmed/25916994
Estrogen's Effects on Yeast Infections
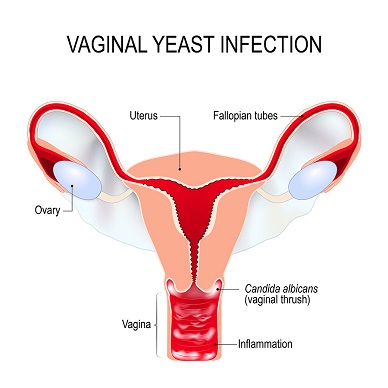
In a scientific study done in 1999 by Paul L. Fidel Jr., Jessica Cutright, and Chad Steele of Louisiana State University, and published in the American Society of Microbiology in 2000, they found that progesterone has no effect on vaginal Candida in mice but excess estrogen promoted its growth. They also found that excess estrogen reduced the ability of vaginal epithelial cells to prevent colonization of Candida on the vaginal walls.
A study published in June 2015 in Current Infectious Disease Reports talks about pregnancy-related factors such as excess estrogen, increased vaginal glycogen levels, and reduced immune function increasing the yeast infection rate of pregnant women. 1
This study in 2006 done by Georgina Cheng, Kathleen M. Yeater, and Lois L. Hoyer with Department of Pathobiology at the University of Illinois, found that elevated estrogen levels and the incidence of vaginal candidiasis are positively associated. The study noted; "The addition of 17-β-estradiol or ethynyl estradiol to Candida albicans cells caused an increase in the number of cells. The transcriptional profile of estrogen-treated C. albicans cells showed increased expression of CDR1 and CDR2 across several strain-estrogen concentration-time point combinations, suggesting that these genes are the most responsive to estrogen exposure".
Basically, "The addition of 17-β-estradiol or ethynyl estradiol to Candida albicans cells caused an increase in the number of cells. In addition, presence of estrogen led to increase in germ tube formation (filamentous growth) in C. albicans; with this form, the yeast anchors to the vaginal wall more easily and colonizes rapidly".
A study in 2000 by Xiaoqian Zhang, Michael Essmann, Edward T. Burt, and Bryan Larsen at the Infectious Disease Research Laboratory in Des Moines Iowa, determined that higher estrogen levels lead to increased growth and survival rates of Candida yeast, which proves that once Candida yeast colonizes the vagina, it becomes hormone-dependent. In addition, estrogen increased the amount of multi-drug resistant Candida rna compared with cells not treated with estrogen.
Dr. Shalaka Samant, PhD says...
Candidiasis appears to occur more often in the setting of increased estrogen levels (3), such as oral contraceptive use (4) (especially when estrogen dose is high), pregnancy, and estrogen therapy. Increased estrogen facilitates adherence of yeast (5) to vaginal mucosal epithelial cells. In addition, estrogen promotes hyphae formation and enzyme production in Candida, which are important virulence factors (6) further enhancing colonization. Therefore, elevated estrogen appears to be an environmental signal (7) for enhancing yeast virulence thereby favouring recurring yeast infections.
3.
Candida vulvovaginitis. Author: Jack D Sobel, MD. Section Editors:
Robert L Barbieri, MD, Carol A Kauffman, MD Deputy Editor: Kristen
Eckler, MD, FACOG. Oct 12, 2016.
4. The impact of oral contraception on vulvovaginal candidiasis. Contraception. 1995 May;51(5):293-7.
5. Vulvovaginal candidosis. Sobel JD1. Lancet. 2007 Jun 9;369(9577):1961-71.
6.
The epidemiology, pathogenesis, and diagnosis of vulvovaginal
candidosis: a mycological perspective. Crit Rev Microbiol. 2011
Aug;37(3):250-61. doi: 10.3109/1040841X.2011.576332. Epub 2011 May 20.
7.
Xiaoqian Zhang, Michael Essmann, Edward T. Burt, Bryan Larsen, Estrogen
Effects on Candida albicans: A Potential Virulence-Regulating
Mechanism, The Journal of Infectious Diseases, Volume 181, Issue 4,
April 2000, Pages 1441–1446
Estrogen Dominance and Other Hormones
What can cause our hormones to be imbalanced? STRESS!
Stress makes the adrenal glands go into overdrive, which causes the body to divert progesterone to the adrenals to support cortisol production. This process reduces progesterone levels and because progesterone offsets estrogen, the body may experience estrogen dominance, i.e. PMS, hot flashes, night sweats, migraines, fibroids, heavy bleeding, breast tenderness, weight gain, etc.
The adrenal gland contributes about 35 percent of premenopausal female hormones and compromised adrenal function profoundly affects hormonal balance.
Excessive cortisol blocks your progesterone receptors, further contributing to low progesterone and progesterone is the primary material for producing cortisol. When progesterone levels go down, estrogen levels rise. Its a big intertwined circle. These two imbalances, excessive cortisol and low progesterone, lead to estrogen dominance. Restoring adrenal function is a required for hormonal balance.
Excessive estrogen levels have been linked to breast cancer and reduced function of the Thymic gland. The Thymic gland helps immune system t-cells that are grown in the bone marrow mature. At a certain stage of t-cell growth in the bone marrow the t-cells migrate to the Thymic gland to mature. Upon maturity of the t-cells, the Thymic gland releases them into the body. So excessive estrogen also affects T cell maturation and immune response.
Chronic low blood pressure can be a key symptom of adrenal exhaustion as well as extreme fatigue or Chronic Fatigue Syndrome, irritability, inability to concentrate, frustration, insomnia, addictions to either sweet or salty foods, allergies, nervousness, depression, anxiety, PMS, sensitivity to cold, diabetes and headaches.
The continued stress and resulting release of cortisol eventually burns out the adrenals and levels quite often crash in the mornings. This study published in 2005 by Ehrström SM and Associates from the Department of Obstetrics and Gynecology in Stockholm Sweden, determined that these low cortisol levels definitely contributed to recurrent vaginal candida yeast infections.
Individuals who suspect adrenal exhaustion can determine whether the body is producing healthy levels of adrenal hormones through proper testing. Cortisol levels can be measured with a saliva test that measures cortisol levels at four different times of the day. If the test shows low cortisol then your adrenals are exhausted and this must be corrected before you can balance all other hormones.
If you determine that you do have an exhausted adrenal glands, you can take Adrenal Stress End and use Progesterone cream to restore the adrenal gland function.
Dr. Shalaka Samant, PhD says...
Estrogen controls critical functions such as glucose homeostasis, lipid homeostasis, bone metabolism, brain function, follicular growth, skeletal growth, and ovulation among a myriad of other functions. Estrogen is a master regulator, (8) and it interacts with a spectrum of other hormones, and enzymes to mediate its versatile functions. Therefore, both hyper and hypo level of estrogen sets off a diverse array of diseases i.e. autoimmune, metabolic, neural, and gender-specific, among others.
8. Estrogen: The necessary evil for human health, and ways to tame it. Biomed Pharmacother. 2018 Jun;102:403-411. doi: 10.1016/j.biopha.2018.03.078. Epub 2018 Mar 22.
Too Much Estrogen Can Affect the Thyroid Gland
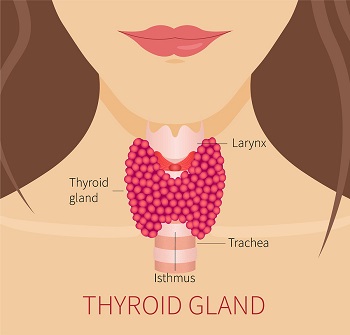
Adrenal exhaustion can lead to Hypothyroidism, which is defined as a low performing thyroid. The most common symptoms are unwanted weight gain, depression, low energy, cold intolerance, thinning hair, sleep disturbance, fatigue, mood swings and a low sex drive.
In his book, What Your Doctor May Not Tell You About Menopause, Dr. John Lee discusses how it became apparent that the taking of thyroid supplements among his women patients was especially common in those with too much estrogen. This is because, when estrogen is not counter balanced with progesterone, the estrogen builds up and blocks proper thyroid function creating hypothyroidism.
More information on Problem Thyroid here.
If you suffer from PMS you can also test your thyroid yourself to get a better idea if you have too much estrogen or not. What you do is take your temperature first thing in the morning before you get out of bed. If it is under 97.5 your thyroid is under performing and it could be because of too much estrogen.
Heavy Metals Can Effect Hormone Levels
Excess mercury can also lead to adrenal and thyroid
problems not
to mention the effect it has on the production of yeast. Mercury is a
hormone disruptor and will have an effect on all your hormones. Its also
been found that candida yeast is 67% more prevalent among people with
amalgam dental fillings than those without.2
You can test your mercury levels yourself with an in home Mercury Test Kit.
If your levels are to high, you will have to be treated by following the directions on the Treatment for Mercury Poisoning webpage.
How to Determine if You Have too Much Estrogen
If you suffer from the symptoms of PMS then most likely you have too much estrogen or not enough progesterone.
However, the best way to determine estrogen levels of course is to take a saliva hormone test to detect estrogen dominance.
Saliva hormone testing is the most accurate test with the least amount of false positives. If the test result reveals a low progesterone - estradiol ratio, then you are estrogen dominant.
Please See the Recurring Yeast Infection Webpage to understand how to treat high estrogen levels if you don't have an adrenal or mercury problem.
If you suffer from too much stress which may have caused all these problems to begin with, please see the How To Relieve Stress webpage so you can get it under control.
Dr. Shalaka Samant, PhD says...
Put simply, estrogen dominance is a state in which the body
contains too much estrogen and too little progesterone. Excess estrogen
can stem from increased estrogen production, increased estrogen exposure
in the environment, or improper breakdown of estrogen. These days our
environment and diet have multiple estrogen mimics that increase
exposure to this hormone. Poor gut and liver health due to an
inappropriate diet diminish our ability to adequately breakdown
estrogen. And to compound matters further, stress increases our
production of the hormone cortisol, which then slows down our ability to
get rid of estrogen.
Thus, there are many possible reasons for why a woman is estrogen dominant, as well as multiple factors that can exacerbate estrogen excess. Testing for estrogen dominance followed by diet and lifestyle changes may help achieve the desired hormonal balance and also potentially ward off recurring yeast infections.
Medical Review by Dr. Atmika Paudel, PhD
In support of what has been written above, a recent study has shown that Candida albicans and Candida glabrata colonized well in high estrogen environment. In addition, their biofilm formation and susceptibility to antifungal agents was also affected by estrogen level. Presence of high estrogen level made the yeasts less susceptible to anti-fungal agents and increased the biofilm dispersion. Overall, the study showed that high estrogen level that mimics the level during pregnancy may function to promote the survival and colonization of Candida making them more readily adaptable to the vaginal environment and may even protect them against vaginal environmental conditions that are adverse to the yeasts (1).
As mentioned in the article, stress can aggravate hormonal imbalance. On the other hand, hormonal imbalance can deteriorate mental well-being. However, a proper balance of hormones are required for the overall well-being and deficiency of hormones also have adverse health effects. Therefore we should be careful not to focus too much on reducing the hormones. They have their own functions in the body, and everything should go in balance. We need to keep watch on our symptoms and be aware of the fact that high reproductive hormone estrogen leads to recurrent yeast infections. The above article makes that fact much clearer and easier to understand in a scientific way.
1. Bruna Gonçalves, Nuno Miguel Azevedo, Mariana Henriques, Sónia Silva, Hormones modulate Candida vaginal isolates biofilm formation and decrease their susceptibility to azoles and hydrogen peroxide, Medical Mycology, Volume 58, Issue 3, April 2020, Pages 341–350
Have Any Questions About Estrogen Dominance?
Do you have any questions about estrogen dominance or yeast infections in general? Ask your question here or contact us using the contact page of this website. It is also always a good idea to talk to your doctor as well.
Back to Vaginal Yeast Infection Webpage
Back to Cause of Yeast Infection Webpage
Article References
1. Curr Infect Dis Rep. 2015 Jun;17(6):462. doi: 10.1007/s11908-015-0462-0. Vulvovaginal candidiasis in pregnancy.Aguin TJ1, Sobel JD.
2. Med Arch. 2012;66(6):415-7 The relationship between oral hygiene and oral colonisation with Candida species. Muzurovic S1, Babajic E, Masic T, Smajic R, Selmanagic A
Home Privacy Policy Copyright Policy Disclosure Policy Doctors Store
Copyright © 2003 - 2025. All Rights Reserved under USC Title 17. Do not copy
content from the pages of this website without our expressed written consent.
To do so is Plagiarism, Not Fair Use, is Illegal, and a violation of the
The Digital Millennium Copyright Act of 1998.