- Home
- Oral Yeast Infections
Oral Yeast Infections, Diagnoses & Treatment
Table of Contents
Updated 12/07/2022
Medically reviewed by Dr. Atmika Paudel, PhD - Written by Dr. Shalaka Samant, PhD and Dan Jackowiak Nc, HHP
Dr. Atmika Paudel, PhD says... The information provided in this article about the causes, symptoms, and potential natural remedies for oral yeast infections is medically correct.
Oral yeast infections also known as thrush can cause raised white curd-like patches that may have red borders on the tongue and can infect other mucous-membrane surfaces in the mouth. Scraping can remove these white patches, leaving a bleeding, painful surface.
Thrush is sometimes seen in infants although it is much more frequent in the terminally ill and people over 50 years of age.
Esophageal candidosis is much more prevalent in men than women.
Many times these infections go down into the throat and infect the pharynx or larynx. The most typical symptom is pain when swallowing or a sensation of food sticking in the throat. Hoarseness or altered vocalization will often occur at this point. There can also be a dry irritating cough and pain in the throat.
Dr. Shalaka Samant, PhD says...
Candida species are commensal yeast of the healthy human oral cavity, gastrointestinal tract, and vagina, but they may also cause superficial infection or invasive, life-threatening disease. Oral candidiasis is an opportunistic infection of the oral cavity caused by an overgrowth or infection of the oral cavity by Candida (1). Oral candidiasis is common and under-diagnosed among the elderly, particularly in those who wear dentures, and in many cases is avoidable with a good mouth care regimen.
The most common causative agents of oral candidiasis are C albicans (the commonest), C tropicalis, C glabrata, C pseudotropicalis, C guillierimondii, C krusei, C lusitaniae, C parapsilosis, and C stellatoidea. C albicans, C glabrata, and C tropicalis represent more than 80% of isolates from clinical infection (2). Commonly known as oral thrush, these infections are characterized by extensive white raised patches in the oral cavity consisting of host epithelial cells, fibrin, and fungal hyphae.
1. Candidiasis of the oropharynx and esophagus. Ear Nose Throat J. 1988 Nov;67(11):832, 834-6, 838-40.
2. Pathogenesis and treatment of oral candidosis. J Oral Microbiol. 2011; 3: 10.3402/jom.v3i0.5771.
Diagnosing Oral Yeast Infections
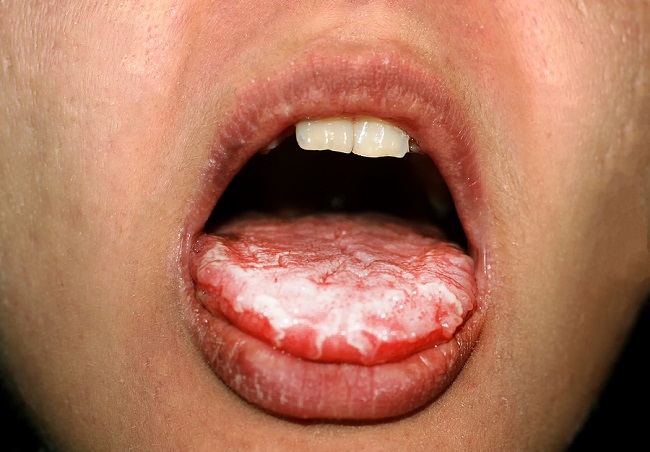
Oral thrush on tongue caused by Candida fungus.
For Esophageal candidosis or oral yeast infections in the throat, an endoscopy is the best method to make a firm diagnosis because the ulcer will be plainly visible. If an ulcer is visible it can be biopsied for a positive diagnosis.
Another diagnostic method is for your doctor to scrape the lesion and view the sample under a microscope. If hyphae or spores are seen then it is yeast.
Scraping the infected area and then sending the sample to a lab for a culture can be used
to determine the species, but most cases of esophageal candida are caused
by Candida albicans or Candida tropicalis.
Tongue thrush can also appear yellowish as shown in this picture. Other oral yeast infection pictures can be found here, including pictures of yeast infections in the throat.
Look in the mirror with your tongue stuck out, if it is heavily coated with a white film, chances are you have an oral yeast infection. However, bad bacteria can also cause this condition so it might be a good idea to see a doctor and have them perform a culture to verify if it is yeast related or not.
If you have bad breath and also the white coated tongue, it is bad bacteria and not yeast. Yeast does not smell bad, bacteria does.
Sometimes these infections will also be found in the intestine. This webpage provides information on testing for yeast so you can determine if you might also have this in your intestine.
Dr. Shalaka Samant, PhD says...
Diagnosis is usually straightforward as it is easily seen by naked eye. Diagnosis can be confirmed microbiologically either by staining a smear from the affected area or by culturing a swab from an oral rinse.
What Causes Oral Yeast Infections
- Diabetes, leukemia and AIDS are common risk factors.
- The use of steroid inhalers and people that wear dentures are also at a higher risk.
- People with mercury dental fillings are 67% more likely to get oral yeast than those without them.
- Thrush infections have been linked to a defect in the white blood cells or a confirmed low white blood cell count.
- Oral sex with an infected male or female.
Low IgA immunoglobulin counts are also highly suspect since this is the immunoglobulin responsible for the defense of the mucousal linings in the body. IgA deficiency is also the most common immune system deficiency seen in humans, and it is usually for life. I suspect this is one of the primary causes of oral yeast infections and many yeast infections in general.
Dr. Shalaka Samant, PhD says...
A change from the harmless commensal existence of Candida to a pathogenic state can occur following alteration of the oral cavity environment to one that favours the growth of Candida. Most often these changes relate to weakening of the host’s immune defences. Antibiotics can predispose to oral yeast infections by removing protective bacterial flora (3), creating an environment that is more conducive to the growth of Candida.
Inhaled steroids, particularly fluticasone, used in therapy for asthma, can increase risk for oral candidiasis by suppressing immune response. 50%–65% of people who wear removable dentures are also predisposed to developing oral candidiasis (4).
Impaired salivary gland function or medications such as antihistamines which can reduce salivary secretion can predispose to oral candidiasis (5). A variety of nutritional factors including deficiencies of iron, folic acid, vitamins, and diets rich in carbohydrates have been implicated in the pathogenesis of oral candida infections (6). Other predisposing factors include smoking, diabetes mellitus, Cushing's syndrome, malignancies, and immunosuppressive conditions.
3. Akpan A, Morgan Oral candidiasis Postgraduate Medical Journal 2002;78:455-459.
4. The prevalence and intra-oral distribution of Candida albicans in man. Arch Oral Biol. 1980;25(1):1-10.
5. Oral candidiasis. Clin Geriatr Med. 1992 Aug;8(3):513-27.
6. Nutritional factors and oral candidosis. J Oral Pathol. 1986 Feb;15(2):61-5.
Medications for Oral Yeast Infections
Nystatin or sometimes Fluconazole is typically used to treat oral yeast infections.
Amphotericin B lozenges would be worth trying if Nystatin and Fluconazole are not effective medications. Doctors de Vries-Hospers HG, Mulder NH, Sleijfer DT, and van Saene HK found them to be very effective for neutropenic leukemia patients with oral candida yeast infections.
Other medications include Mycelex Troche or Clotrimazole, Itraconazole, and Posaconazole for people that are over 13 years of age.
It is best to send a culture from your mouth to a lab so the lab can determine what kills the yeast. That way your doctor can prescribe the most effective medication the first time.
Dr. Shalaka Samant, PhD says...
Management of oral candidiasis typically involves a prescription of topical antifungals such as nystatin for two weeks. In certain high risk groups antifungal prophylaxis reduces the incidence and severity of infections. Prophylaxis with antifungal agents reduces the incidence of oral candidiasis in patients with cancer undergoing treatment also. The prognosis is good for oral candidiasis with appropriate and effective treatment. Relapse when it occurs is more often than not due to poor compliance with therapy (7), failure to remove and clean dentures appropriately, or inability to resolve the underlying/predisposing factors to the infection.
7. Oral candidiasis: pathogenesis, clinical presentation, diagnosis and treatment strategies. J Calif Dent Assoc. 2013 Apr;41(4):263-8.
Treating Oral Yeast Infections Naturally
Below is a list of medically proven natural products for treating oral yeast infections caused by candida yeast. Studies can be accessed from the Herbal Remedy page here.
It will be an experiment to find what works the best because not every species of yeast is susceptible to the same anti-fungal herbs or drugs for that matter.
Gentian Violet has been found to work well against oral and skin Candida yeast infections. It also has antimicrobial activity against certain species of bacteria. You can learn more about Gentian Violet here.
Candidate is an herbal product that contains pau d'arco that is medically extracted in a tincture form. Laboratory tests have demonstrated that pau d'arco's anti-fungal properties are as potent as ketoconazole. It also contains lemon grass and Calendula officinalis which are proven anti-fungals that stimulate the immune system, repair the lining in the intestine, and are very good for the liver. Apply the drops directly to the thrush or dissolve in a little water and swish as long as possible before swallowing.
Pau d'arco can also be used by itself in tincture form or teas. Drops should be applied directly to the lesions and it would be best to swish and swallow with the tea.
Cinnamon oil for yeast infections has been found to be deadly to drug resistant candida yeast and other fungal infections. The active ingredients are cinnamaldehyde, linaaol and eugenol. Preliminary human evidence confirms this effect in a clinical trial with AIDS patients suffering from oral candida (thrush) infections that improved with topical application of cinnamon oil. Antibacterial actions have also been demonstrated for cinnamon oil concentrates. The diterpenes in the volatile compound have shown anti-allergic activity as well. In addition, water extracts may help reduce ulcers. Apply directly to the thrush or dilute in a tbsp of coconut oil and let dissolve in your mouth.
Oregano oil for oral yeast infections has been tested extensively against molds, yeast, fungi, and candida in the scientific field. It is a proven candida yeast killer and the best results are achieved when the oregano oil contains 68.1% or more of carvacrol, which is the active ingredient in the oil. Apply directly to the thrush or dilute in a tbsp of coconut oil and let dissolve in your mouth.
Grapefruit seed extract in liquid form
is another medically proven candida yeast killer. You can use it
straight on the spots or add it to a little coconut oil if it's to hot.
Coconut oil for treating oral yeast explodes the nucleus of the yeast cell and is also good for treating intestinal or skin infections. Just take a tbls by mouth and hold in your mouth until it dissolves before swallowing. It also works well for skin yeast by applying directly on the infection.
Colostrum provides IgA antibodies and immunoglobulins that help the immune system. Chewable forms are the best to take whether treating oral thrush because you must let this dissolve in the mouth for any positive effects.
Another option that people are having good success with, is Biofase and Profase
mixed together and sprinkled on the tongue. Then move it around in your
mouth for as long as you can before rinsing it down with water.
Dr. Shalaka Samant, PhD says...
In vitro studies of probiotics, such as Lactobacillus acidophilus, Bifidobacterium bifidum, and L. rhamnosus, have demonstrated that they reduce the virulence of Candida by inhibiting biofilm formation and may provide additional benefit to antifungals (8). Studies of probiotics in patients with dentures (9) who are also at increased risk for candidiasis have likewise shown promising results.
8. Probiotics for oral and vulvovaginal candidiasis: A review. Dermatol Ther. 2019 Jul;32(4):e12970. doi: 10.1111/dth.12970. Epub 2019 May 30.
9. A multispecies probiotic reduces oral Candida colonization in denture wearers. J Prosthodont. 2015 Apr;24(3):194-9. doi: 10.1111/jopr.12198. Epub 2014 Aug 20.
Medical Review by Dr. Atmika Paudel, PhD
The article is well-written covering the overall picture of oral yeast infections and is supported with evidence-based literature. Like the article mentioned, oral yeast infections can occur to people of any age group, from infants to elderly.
Usually, Candida albicans is the causative agent or oral yeast infection, which is also called as oral thrush. C. albicans normally reside in the gastrointestinal tract as a commensal, but in an event of decreased immunity and microbiome dysbiosis, they overgrow and invade the tissues. Several of the predisposing factors include prolonged use of broad-spectrum antibiotics, immunosuppressive agents, or devices such as dentures that can be a suitable place for the yeast to form biofilm and persist (1).
While oral thrush is common, they are diagnosed pretty quickly without a delay in treatment. As soon as we feel some pain, or see the white patches over our tongue, we will speculate that it is the oral thrush and rush to the hospital or to see our doctor. Because it will profoundly affect our daily life, with a feeling of something inside your mouth all the time, with you not being able to enjoy the taste of foods, and difficulty in swallowing the food, the constant uneasiness promotes early hospital visits. If it is treated and you are recovered, you will feel a lot better. However, if you get oral thrush recurrently, you need to consider other ways in order not to let it happen again and again.
Use of antifungal agents are okay but their long-term use is not good either. You have to boost your immunity of the body so that your body itself can fight with the yeast and let it not infect you again. Recurrent oral thrush can cause the infection to spread to internal organs. So, boosting your immunity and keeping your microbiome balanced is the key.
- Vila T, Sultan AS, Montelongo-Jauregui D, Jabra-Rizk MA. Oral Candidiasis: A Disease of Opportunity. J Fungi (Basel). 2020 Jan 16;6(1):15. doi: 10.3390/jof6010015. PMID: 31963180; PMCID: PMC7151112.
Have Any Questions About Oral Yeast Infections?
Do you have any questions about oral yeast infections or yeast infections in general? Ask your question here or contact us using the contact page of this website. It is also always a good idea to talk to your doctor as well.
Questions From Other Visitors
Click below to see questions from other visitors to this page...
What can I do to be proactive for oral yeast ? 




Hi Dan,
I have mild asthma now and take a steroid inhaler. I rinse and brush my teeth right right after using the inhaler. I have a constant bad taste …
Oral Yeast Infection Testimonials
Hi Dan,
I just wanted to let you know that opening the biofase and profase and putting it on my tongue the last couple of days has performed wonders. All of the white on my tongue has gone away! My tongue is back to its normal pink color and it does not sting like it has been. I have been struggling with thrush for the last 6 months now, so I just want to say thank you so much for your advice!!
I had tried everything under the sun and spent thousands of dollars and nothing has worked, which has been so frustrating for me. So the fact that I am seeing results and my tongue is back to normal makes me so happy and finally feel like everything I have been doing is worth it now!
Sincerely,
Maleah
*****
Hi Dan,
Biofase is Wonderful!
I
am using Biofase in conjunction with caprylic acid/ psyllium/
bentonite. I am also using it in another way I thought you might like
to know about. I emptied a capsule and put in on the back and sides of
my tongue to see if it would dissolve the film. The next day the sides
were clear and the back was a little better. I follow it by pulling
coconut oil and caprylic acid through my teeth and letting it coat my
tongue for 15 minutes. It seems to do the trick. It does NOT taste
good, but desperate people try desperate things. I love seeing my
almost clear tongue in the morning. And that tinny taste that stays
with me is almost gone. I thought you might like to know.
Update two weeks later.
I found that if Biofase is placed directly on the tongue, it works well,
but irritates the throat and roof of the mouth. It is better to make it
into a thin paste with water and coat the tongue, leaving it on for 10
minutes. It is not quite as effective, but gentler on the rest of the
mouth. Still, my tongue looks great!
Michelle
*****
Dear Dan,
Please allow me to tell it like it is or WAS !! Oral candidis can be compared to unstoppable cancer or in my case I felt like a leper! Not a spot in my mouth or throat where I was not being eaten alive. Barely able to swallow pureed foods. Fluconazole saved me, but after several relapses, I asked by Dr. what would happen if my body resisted the drug. He said "You're out of luck"! I soon became resistant and I was out of luck for sure... that is until I found yeastinfectionadvisor.com.....a gift from God, an answer to a prayer for help....I was saved again with Syntol, Latero and 11 strain but remained on constant guard because for me those weapons only held the enemy at bay. In comes Biofase to the rescue!! Believe me, 6 Biofase can do what 8 Syntol can not do...the enemy is dead...I am free at last and am in the maintenance phase with Biofase, Latero, and 11 Strain. I really appreciate your keeping the Biofase cost down!
God Bless you Dan,
Anthony
*****
Hi Dan,
I
just wanted to say thanks - I have recently had tests for candida and I
am all clear thanks to your regime. My geographic tongue is much much
better but I will now be looking closely at my vitamin and mineral
levels to try and sort out the rest of this conundrum.
I will be staying on the diet for the the foreseeable future as I feel so
much better and my sleeping pattern is much improved.
With kind regards and thanks again for all your great emails and
encouragement.
Lynda
If you tested your stool for the presence of yeast in your intestine and it was positive, I highly recommend you do the entire yeast infection treatment system. Yeast infections in two or more places are considered chronic infections and are best treated as such.
Systemic Yeast Infection Treatment
Home Privacy Policy Copyright Policy Disclosure Policy Doctors Store
Copyright © 2003 - 2025. All Rights Reserved under USC Title 17. Do not copy
content from the pages of this website without our expressed written consent.
To do so is Plagiarism, Not Fair Use, is Illegal, and a violation of the
The Digital Millennium Copyright Act of 1998.