- Home
- Herbal Remedies
- Uva Ursi for Uti
Uva Ursi for Uti & Yeast Infections
Posted 2/5/2020
Written By Pharmaceutical Scientist Dr. Harmeet Kaur, PhD
This
article talks about Uva Ursi's effects on yeasts, bacteria, its other
uses and health benefits, and possible safety issues and side effects.
Uva ursi for uti (Arctostaphylos uva ursi), also called bearberry (as a favorite food for bears), is a trailing evergreen shrub, that flourishes in the temperate soil of Europe, North America, and Asia. This plant has medicinal importance since the 2nd century. Although its red berries are edible, the dried leaves are the only part of the plant which are used as traditional medicine as a diuretic, antimicrobial, and anti-inflammatory agents for various diseases especially of the urogenital tract and mild kidney infections. Actually, until the discovery of sulfa drugs and antibiotics, Uva ursi was a conventional treatment for bladder-related infections [1,2].
Chemical Constituents of Uva Ursi
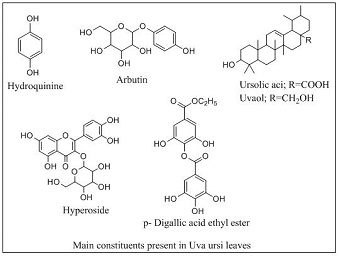
The primary constituents present in leaves of Uva ursi for uti are phenolic glycosides as arbutin (5-15%), methylarbutin (up to 4%) and related derivatives such as hydroquinone. The leaves also contain gallic acid as the significant phenolic carboxylic acid, together with galloyl arbutin and up to 20% of gallotannins; flavonoids such as hyperoside (1.3%) mainly the flavonols kaempferol, quercetin, and myricetin and their glycosides, quercitrin, isoquercitrin, hyperin, and myricitrin; and triterpenes, mainly ursolic acid and uvaol.
Recently, Kurkin et al. found new natural compound p-digallic acid ethyl ester and the other compound 1,3,6-trigalloylglucose in the leaves of Uva ursi. Leaves also contain trace minerals like iron, manganese, silicon, selenium, organic acids, vitamins and other secondary plant metabolites [3,4].
Role of Uva Ursi as an Antimicrobial Agent
From times of ancient Egypt up to the early 19th century, the herbal plants of medicinal importance have mainly envisioned for the treatment of urinary tract infections (UTIs). With time, these herbal treatments replaced by more selected and active antimicrobial agents; however, the frequent and irrational use of antimicrobial agents in the prophylaxis and therapy has led to the emergence of antibiotic-resistant uropathogens. This has triggered an interest in the plant-derived antimicrobials for prevention and control of UTIs. Uva ursi is one of the medicinal plants reconsidered for use in UTIs [5].
The crude
leaf extract and arbutin, the active antimicrobial ingredient in Uva
ursi for uti both have shown in vitro bacteriostatic activity against
Gram-positive (Bacillus subtilis), and Gram-negative (Enterobacter, E. coli, Helicobacter pylori, Shigella sonnei, Shigella flexneri and Klebsiella) bacteria [6]. These bacteria are the main causative agents responsible for UTIs.
Arbutin also repressed the expression of a critical virulence factor for Listeria monocytogenes,
which causes febrile gastroenteritis, perinatal infection and systemic
infections of the central nervous system [7]. Schindler et al. (2002)
conducted a study with human beings which have taken dried leaf extract
of Uva ursi as tablets and in aqueous solution form. Approximately 64.8%
of arbutin from tablet and 66.7% of arbutin from aqueous solution are
released in the urine attributing to its antimicrobial action [8].

Frohne (1970) and Kedzia et al. (1975) evaluated the urine of patients for antimicrobial activity who have consumed extracts of Uva ursi for uti or isolated arbutin. The urine from the treatment group has demonstrated significant antimicrobial activity against P. mirabilis, E. coli, S. aureus, P. aeruginosa and 70 other urinary bacteria [9,10]. Frohne (1970) also established that the crude extract of Uva ursi was more effective as compared to arbutin by itself.
On oral administration, arbutin breaks down in the human system by hydrolysis to form hydroquinone, a powerful disinfectant. Toxic hydroquinone then combines with glucuronic acid or sulfate and is excreted through the kidney in the conjugated form, but on the other hand, when leaves of Uva-ursi are used as a crude drug, gallotannin (gallic acid) present in leaves prevents enzymes from splitting arbutin and hence increases the effectiveness of Uva ursi leaves [11].
Larsson et al. (1993) conducted the clinical studies to investigate the therapeutic efficacy of Uva ursi for uti in management of UTIs by utilizing a combination extract of Uva ursi with dandelion Taraxacum Officinalis which involved double-blind, placebo-controlled, randomized trial of 57 women with chronic UTIs for one month and subsequently followed for a year. Significantly more women in the placebo group experienced recurrent cystitis compared to the treatment group, thereby demonstrating the efficacy of Uva ursi as an antimicrobial for the treatment of UTIs [12].
The antimicrobial effects of Uva ursi are due to its constituents, particularly quinones, which form an irreversible complex with the nucleophilic amino acids present in proteins. They are also believed to affect surface-exposed adhesins, cell wall polypeptides, and membrane-bound enzymes and change microbial cell surface characteristics and hence adhesion of' microbes on host cells which is a critical factor in the development of Gram-negative microbe-induced infections [13].
A study by Turi et al. (1997) has also proved that in the presence of Uva ursi for uti extracts the growth of clinical isolates of E. coli augmented the microbial cell surface hydrophobicity, thus decreasing their ability to adhere to host cells [14]. Flavonoids are synthesised by plants, partly in response to microbial infection. Therefore, it is not surprising that flavonoids may at least be partially responsible for the antimicrobial activity of many plants. Both flavonoids and tannins believed to act like quinones.
Furthermore, Uva ursi for uti has diuretic and anti-inflammatory effects that indirectly aid in its use as an antimicrobial to control UTIs [15,16] The antiseptic effect of Uva ursi reported to be more active in alkaline urine, and therefore ingesting foods (like fruits and vegetables and reduction of animal proteins) or compounds such as sodium bicarbonate, which can increase pH of urine, has often been suggested in order to enhance its activity. A recent study, though, on the bacterial deconjugation of arbutin by E. coli suggests that alkalization of the urine is not a prerequisite for increasing the antiseptic properties of hydroquinone released from arbutin. Moreover, some UTIs (e.g., those caused by Proteus mirabilis) only occur at alkaline pHs. Thus, alkanalize the urine without identification of the causative pathogen, such as in self-medicating or treating without appropriate urinalysis, may not be suitable for some UTIs [17,
18].
Uva Ursi Works Against Fungi & Yeasts
Tannins present in Uva ursi for uti have reported eliciting antimicrobial activity against filamentous fungi, yeasts, and bacteria. The tannins also have used for controlling schistosomiasis in humans by controlling the disease-transmitting snails [19].
Arbutin and its metabolites also inhibited the in vitro growth of Mycoplasma hominis, Pseudomonas aeruginosa, and Ureaplasma urealyticum. The Commission E of the German Federal Institute for drugs and medical devices (the agency which assesses the effectiveness and safety of herbal products) have also approved Uva ursi for treating inflammation of the lower urinary tract.
The Uva ursi for uti leaf extract also has demonstrated good antifungal activity against Candida albicans which causes illness of varied severity from skin disease, thrush (mouth and vagina), digestive disorders such as crohn's disease, depression, autoimmune disease, some cancers and genitourinary candidiasis.
The tannins and steroidal triterpenes are the main constituents in Uva ursi leaves for the antifungal activity. Mycetoma is a chronic fungal infection of skin tissues caused by devastating fungus Madurella mycetomatis which shields itself against the existing antifungal drugs by the production of melanin, resulting in decreased effectiveness of antifungal drug therapy. Omer and Eltayeb found both arbutin powder and Uva ursi leaf extract decreased the melanin synthesis by Madurella mycetomatis and hence can be used with current antifungal drugs for optimization and potentiation of effect towards mycetoma [20,21].
In addition, Uva Ursi is always tested against all pathogens found on the stool tests we recommend. Most of the time, it is found to be an effective agent against pathogenic bacteria and yeasts of all species.
Uva Ursi for Uti Side Effects
Uva ursi for uti is safe for most adults when taken short-term. The reported side effects from the ingestion of dried Uva ursi leaves include nausea, vomiting, insomnia, irritability, and an increased heart rate. Extremely high doses can cause shortness of breath, ringing in the ears, convulsions, delirium and collapse. Uva ursi has also been linked to, hematuria, albuminuria, eye problems and liver damage with long-term use. Due to its tannin and hydroquinone content, Uva ursi is not suggested for patients with severe renal or hepatic disease or gastrointestinal irritation. The use of uva ursi during pregnancy is likely unsafe because it might start labour [22].
Uva Ursi for Uti Dosage and Duration
The recommended dose of Uva ursi for uti is 2-4g/day as a dried herb standardized to a total of 400-800 mg of arbutin. It can also be consumed in the form of tea or tincture. Steep 3 g in 150 ml boiling water for 15 minutes, up to four times daily, corresponding to 400-840 mg arbutin per day. The herbal plant containing arbutin should not be taken for more than a week or exceed five times a year without a physician consultation [23].
Interactions:
The different formulations of Uva ursi for uti should not be taken with any substances that cause acidic urine such as vitamin C or citrus fruits since they can reduce the antibacterial effect. An alkaline pH should be maintained by consuming a diet rich in vegetables (especially tomatoes), fruits and fruit juices, potatoes, etc.
To conclude:
Uva ursi for uti has used as medicine to treat urinary tract infections (UTIs) and cystitis (bladder inflammation) for the past 700 years. The arbutin is the active constituent present in Uva-ursi leaves and its breakdown in the body forms hydroquinone, a disinfectant. Based on new historical use, Uva ursi appears to be a relatively safe herb when ingested in the amounts typically recommended and used for a limited time.
About the Author

Dr. Harmeet Kaur received her Bachelors in Pharmacy from Guru Nanak Dev University in Amritsar, India in 2000. Guru Nanak Dev University is a state owned university with an "A" grade nationally.
Dr. Kaur received her Masters in Medicinal Chemistry from the National Institute of Pharmaceutical Education and Research in 2002.
In 2015 Dr. Kaur was awarded her Ph.D in Pharmaceutical Sciences from Maharshi Dayanad University in Rohtak, India.
Dr. Kaur is presently a Senior Research Scientist at Maharshi Dayanand University in India.
Dr. Kaur has over 35 published Research papers concerning infectious diseases caused by yeasts, fungi, and bacteria using both prescription drugs and natural plant compounds. She has also performed many studies on cancer cells.
Of particular importance to us, is her multiple experiments performed on Candida albicans and pathogenic bacteria using natural compounds. Because of this experience, we are thrilled to have her on the YeastInfectionAdvisor team.
Back to Herbal Yeast Infection Remedies
Any questions about Uva Ursi for uti or about yeast infections in general, please feel free to contact us from the contact page of this website or talk to your doctor.
Dr. Kaur's References
1.
Geetha RV, Roy A, Lakshmi T. Nature’s weapon against urinary tract
infections. The International Journal of Drug Development and Research
2011;3(3):85-100.
2. Uva ursi. In: LaGow, B, chief editor. PDR for Herbal Medicines. 3rd ed. Montvale, NJ:Thomson 2004; pp. 847-851 ISBN 1563635127
3.
Ștefănescu BE, Szabo K, Mocan A, Crişan G. Phenolic compounds from five
Ericaceae species leaves and their related bioavailability and health
benefits. Molecules 2019;24(11):2046.
4.
Kurkin VA, Ryazanova TK, Daeva ED, Kadentsev VI. Constituents of
Arctostaphylos Uva-ursi leaves. Chemistry of Natural Compounds 2018;54(2):278-80.
5.
Head KA. Natural approaches to prevention and treatment of infections
of the lower urinary tract. Alternative Medicine Review 2008;13(3): 227-244.
6. Wright C. Arctostaphylos uva-ursi, Bearberry.
7.
Park SF. The repression of listeriolysin O expression in Listeria
monocytogenes by the phenolic β‐D‐glucoside, arbutin. Letters in Applied
Microbiology 1994;19(4):258-60.
8.
Schindler G, Patzak U, Brinkhaus B, von Nieciecki A, Wittig J, Krähmer
N, Glöckl I, Veit M. Urinary excretion and metabolism of arbutin after
oral administration of arctostaphylos uvae ursi extract as film‐coated
tablets and aqueous solution in healthy humans. The Journal of Clinical
Pharmacology 2002;42(8):920-7.
9. Frohne D. The urinary disinfectant effect of extract from leaves Uva ursi. Planta Medica 1970; 18:1-25.
10.
Kedzia B, Wrociński T, Mrugasiewicz K, Gorecki P, Grzewińska H.
Antibacterial action of urine containing products of arbutin metabolism.
Medycyna doswiadczalna i mikrobiologia. 1975;27(3):305.
11.
Matsuda H, Nakamura S, Shiomoto H, Tanaka T, Kubo M. Pharmacological
studies on leaf of Arctostaphylos uva-ursi (L.) Spreng. IV. Effect of
50% methanolic extract from Arctostaphylos uva-ursi (L.)
Spreng.(bearberry leaf) on melanin synthesis. Yakugaku zasshi: Journal
of the Pharmaceutical Society of Japan 1992;112(4):276-82.
12.
Larsson B, Jonasson A, Fianiu S. Prophylactic effect of Uva-E in women
with recurrent cystitis: A preliminary report. Current Therapeutic
Research 1993;53:441-443.
13.
Annuk H, Hirmo S, Türi E, Mikelsaar M, Arak E, Wadström T. Effect on
cell surface hydrophobicity and susceptibility of Helicobacter pylori to
medicinal plant extracts. FEMS Microbiology Letters. 1999;172(1):41-5.
14.
Tüuri M, Tüuri E, Kõljalg S, Mikelsaar M. Influence of aqueous extracts
of medicinal plants on surface hydrophobicity of Escherichia coli
strains of different origin. Apmis. 1997;105(7‐12):956-62.
15.
Beaux D, Fleurentin J, Mortier F. Effects of extracts of Orthosiphon
stamineus Benth, Hieracium pilosella L., Sambucus nigra L. and
Arctostaphylos uva-ursi (L.) Spreng. in rats. Phytotherapy Research 1999;13:222–225.
16.
Trill J, Simpson C, Webley F, Radford M, Stanton L, Maishman T,
Galanopoulou A, Flower A, Eyles C, Willcox M, Hay A. Uva-ursi extract
and ibuprofen as alternative treatments of adult female urinary tract
infection (ATAFUTI): study protocol for a randomised controlled trial.
Trials. 2017;18(1):421.
17. Integrated Laboratory Systems Staff. (2006). Chemical Information Review Document for Arbutin and Extracts from Arctostaphylos uva-ursi. National Toxicology Program.
18. Siegers C, Bodinet C, Ali SS, Siegers CP. Bacterial deconjugation of arbutin by Escherichia coli. Phytomedicine 2003;10:58-60.
19.
Wahner C, Schonert J, Friedrich H. Knowledge of the tannin contained in
leaves of the bearberry (Arctostaphylos uva-ursi L). Pharmazie 1974; 29:616-7.
20. Achkar JM, Fries BC. Candida infections of the genitourinary tract. Clinical microbiology reviews. 2010;23(2):253-73.
21. Omer AS, Eltayeb IM. Pharmacognosy and medicinal plants. Journal of Immunology. 2018;179:3065-74.
22.
de Arriba SG, Naser B, Nolte KU. Risk assessment of free hydroquinone
derived from Arctostaphylos Uva-ursi folium herbal preparations.
International Journal of Toxicology 2013;32(6):442-53.
23. Bone, K., Mills, S. (2013) Principles and Practice of Phytotherapy Modern Herbal Medicine, 2nd Edition. Science Direct.com.
Home Privacy Policy Copyright Policy Disclosure Policy Doctors Store
Copyright © 2003 - 2025. All Rights Reserved under USC Title 17. Do not copy
content from the pages of this website without our expressed written consent.
To do so is Plagiarism, Not Fair Use, is Illegal, and a violation of the
The Digital Millennium Copyright Act of 1998.